Geospatial Science Optimizes Polio Eradication Efforts
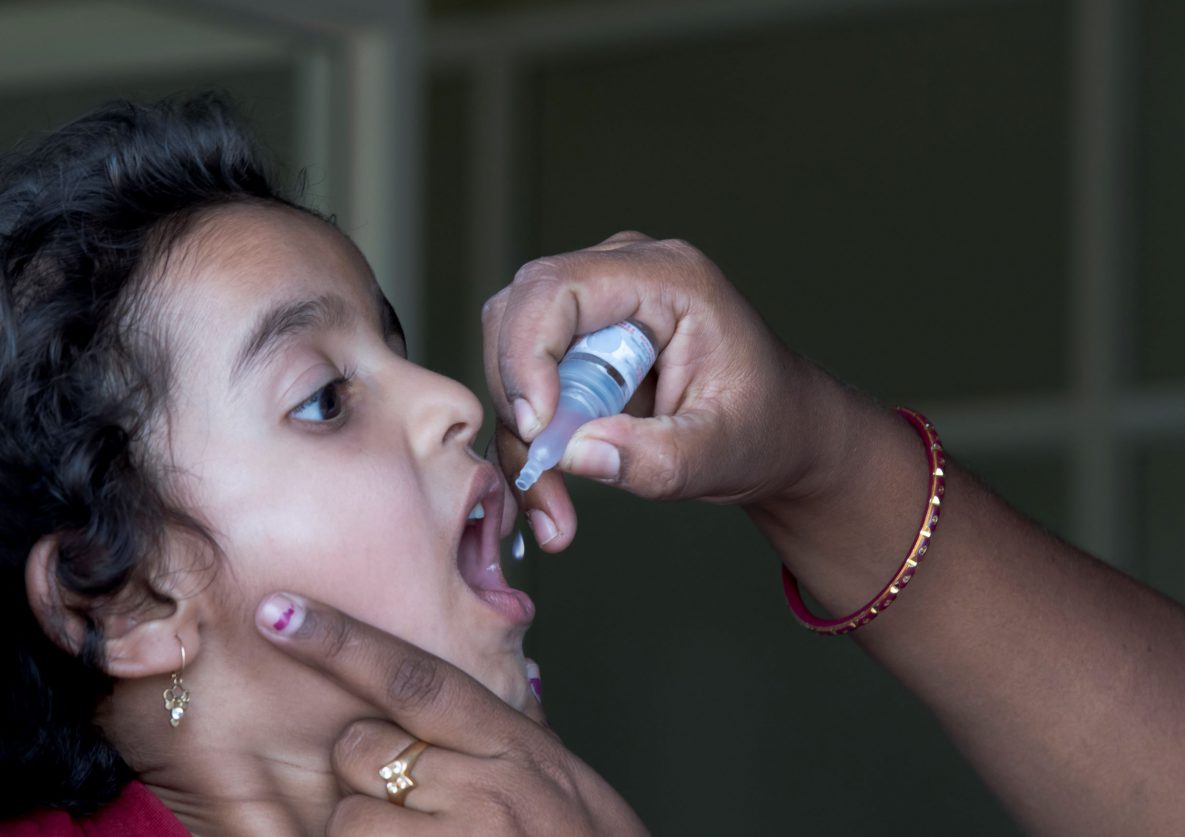
Globally, 20 million children have received incomplete or no life-saving vaccines. Nearly half of them live in countries where conflicts and population displacement make it difficult to reach children with essential vaccinations. When health professionals miss even a single child during polio vaccine campaigns, it can negatively impact global polio eradication efforts.
Working Together
GIS experts and staff from CDC’s Center for Global Health (CGH); CDC/ATSDR’s Geospatial Research, Analysis, and Services Program (GRASP); the World Health Organization (WHO); and Maxar Technologies Inc. collaborated to enhance existing polio campaign efforts by using geographic information systems (GIS) and satellite imagery.
Through this collaboration, a mapathon (community mapping activity) and innovative machine learning technologies were effective tools to improve remote location surveillance and inform logistics and delivery strategies needed to reach children in Central Asia.
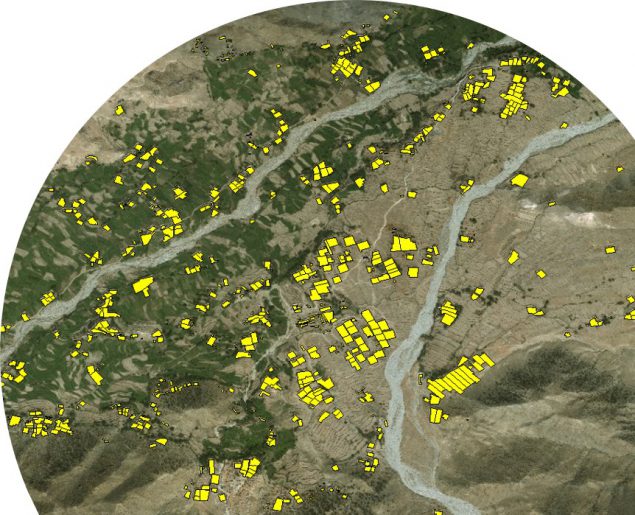
Estimating the number of residential households in hard-to-reach areas is a common challenge for teams executing public health interventions. For example, existing polio vaccination plans include only the houses health professionals can reach, and not abandoned and inaccessible houses.
“GIS expertise and guidance from GRASP team members was essential for us to visualize the geographic distribution of our target populations and to find dwellings that might not be captured on traditional microplans,” says Maureen Martinez, Acting Team Lead for the Eastern Mediterranean Team in CGH’s Polio Eradication Branch.
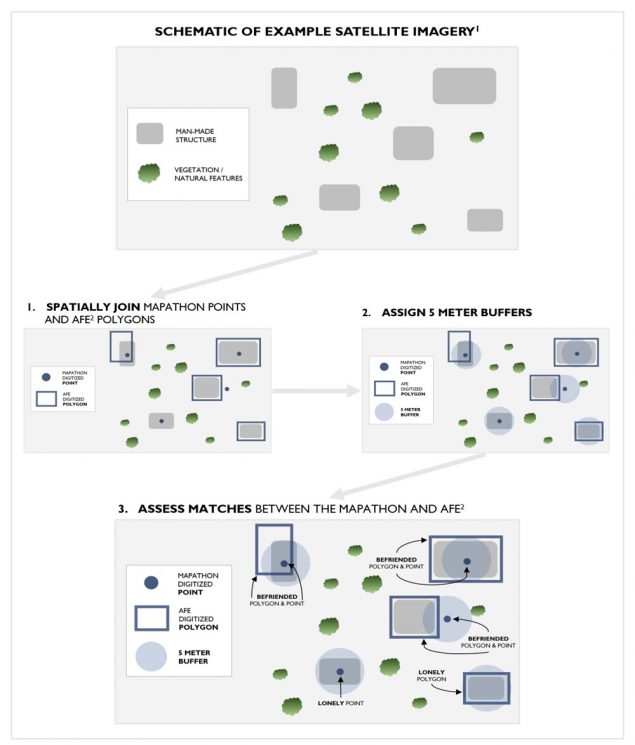
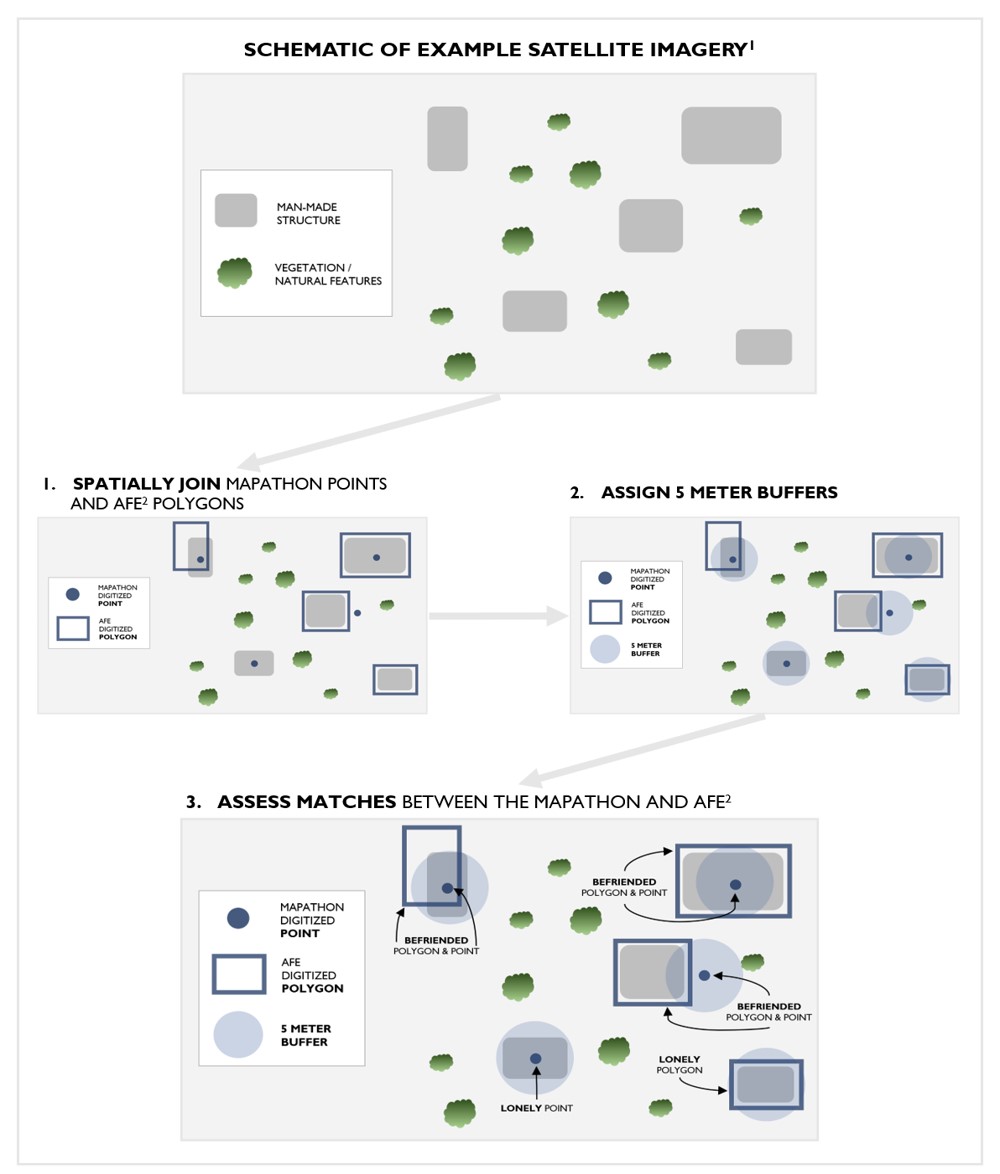
To evaluate the difference in population estimates, staff from GRASP and CGH compared the accuracy and similarity of two GIS methods with existing vaccination campaign plans. Automated Feature Extraction (AFE) and a mapathon yielded up-to-date maps of residential buildings and settlements to the polio response teams. These GIS technology and geospatial methods can improve the remote identification and mapping of vulnerable populations to ensure inclusion in outreach and immunization services, when feasible.
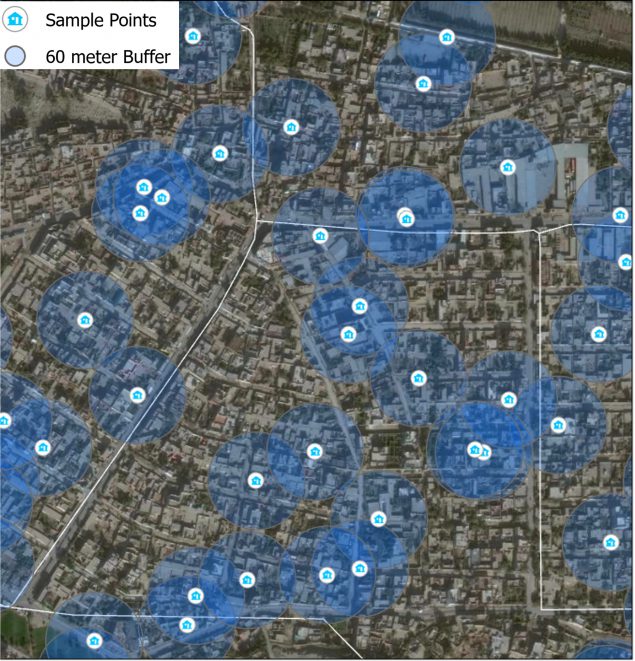
Data Collection – The Tale of Two GIS Methods
The AFE and mapathon methods could be used to benefit other public health campaigns where access to target populations is challenging. The following are key takeaways from using these methods:
- AFE is more accurate in detecting settlements and residential structures when compared to the mapathon.
- AFE is recommended when time constraints exist and areas of interest are large, as this method can speed up the work. However, AFE is a more expensive option than mapathons.
- Mapathons are suggested when areas of interest are smaller and there are no time constraints from the collaborative and participatory nature of the work.
- Both AFE and mapathon methods need to be validated by teams in the field.
While both methods have their advantages, the ideal method would be to use both techniques together to inform public health interventions.
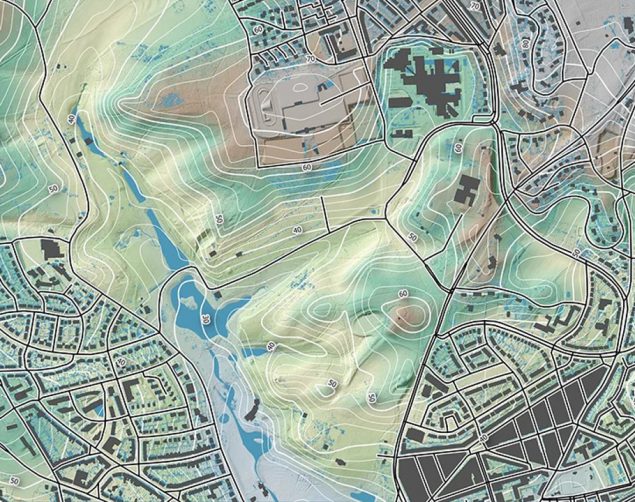
Benefits of Remote Sensing in Public Health
Having up-to-date data in hand allowed the team to optimize logistics and focus their efforts, which was crucial for targeting vaccination efforts, saving time, saving resources, and protecting the lives of field workers in locations where conflict could compromise their security.
As public health professionals work toward vaccinating every child, GIS provides up-to-date information and critical data about where families are located and estimates of how many children are waiting for their polio vaccination, which is a crucial step to eradicate polio.
Read more about this work in the manuscript, Mapathons versus automated feature extraction: a comparative analysis for strengthening immunization microplanning, available online at the International Journal of Health Geographics.